Disclaimer: This article/website
does not provide medical advice. The information, including, but not limited to
text, graphics, images and other material contained on this blogsite are for
informational purposes only. No material on this site is intended to be a substitute
for professional medical advice, diagnosis or treatment. Furthermore, any/all
contributors mentioned in this article are presenting only ANECDOTAL findings of the effects of the
products/technologies they are featuring- and are not offering clinical data or
medical recommendations in any way. Always seek the advice of your physician or
other qualified health care provider with any questions you may have regarding
a medical condition or treatment and before undertaking a new health care
regimen, never disregard professional medical advice or delay in seeking it
because of something you read on this page, article, blog or website.
The NON-INVASIVE MOVEMENT IN MEDICINE was largely shaped by the clever use light, laser, near-infrared, sonic, magnetism and other electronic emissions to collect vital information on a patient's specific state of health without any cutting or physical intervention. This article reviews today's impressive use of high-speed, quantifiable and accurate data-gathering in our medical technologies.
In a (now) standardized sleep study, patients diagnosed with Sleep Apnea will actually stop breathing 20-30 times per hour- bringing potentially significant health risks like stroke, organ failure and heart disorders like atrial fibrillation. An astounding 18M+ Americans suffer this disorder that health providers are incentivized to call a "must fix".
The clinical society addresses this with a sleep study protocol called
POLYSOMNOGRAPHY, collecting data on the patient's varying brain waves, breathing patterns, blood/oxygen levels, heart rate and breathing and eye, leg and body movements.
But as with many personal consumer health devices, polysomnography inspired the rise of wearable wrist monitors for physical fitness and activity tracking (ie. Smartwatch™, Apple Watch™, Fitbit™ etc). These bio-sensory devices tend to carry a wide variety of popular interactive features from a pedometer to mindfulness tracking as well as vital health metrics including heart rate variability (BPM), blood pressure, Oxygen Saturation (SpO2), breathing rate. Most carry a Sleep Tracker feature, comprised of intelligent collaboration of this data to help the user recognize potential sleep problems or therapy progress[1]. Though not marketed to replace clinical
POLYSOMNOGRAPHY, the
medical-grade ECG (Electrocardiography) or medical checkups anytime soon[1c], they do provide the consumer with preliminary in-home lifestyle support on a supplemental level. The bio-scanning technology comes from photodiodes or PHOTOPLETHYSMOGRAPHY to measure blood flow. These wrist monitors often have red or green sensor lights that scan volume changes in the capillaries above your wrist. [1b] This Optical Scanning Technology is similar to semiconductor diodes except that they may be either exposed (to detect vacuum UV or X-rays) or packaged with a window or optical fiber connection to allow light to reach the sensitive part of the device. [1a]
The concept of health tracking via OST light diodes for data-gathering in medical and consumer health products shows evidence of continued utility trends and growing research.
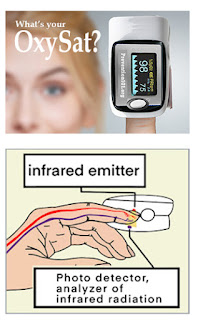
SCANNING VITALS WITH INFRARED:A popular and remarkable example of light emitting diagnostics is THE PULSE OXIMETER – which measures oxygen saturation in peripheral arterial blood by illuminating the skin and measuring the light absorption of oxygenated (oxyhemoglobin) and deoxygenated (reduced hemoglobin) blood using infrared light [2]. The Pulse Oximeter is an electronic device that clips onto a patient’s finger to measure heart rate and oxygen saturation in his or her red blood cells—the device is useful in assessing patients with lung disease. In the first months of the pandemic surge, waves of empty shelves included the widespread purchase of the Oximeter as part of standard home-scanning equipment. This reflects a significant part of "the Covid Culture"- comprising the demand for personal safety measures (beyond the holy trinity of masking, distancing and hand hygiene). The public confidence in this affordable device reflected on its commercial access and data scanning accuracy. In addition, more and more drug store shelves continue to stock up on self-check devices including the hand-held infrared Thermometers, Blood Pressure Cuffs and Spirometers.[3]
THERMAL ENERGY SCANNING WITH INFRARED
The basic premise of scanning temperature readings with infrared is widely useful in various applications including medical diagnostics. INFRARED thermography (IRT), thermal video and thermal imaging captures an impression of any object using infrared radiation emitted by the device to detect radiation in the long-infrared range of the electromagnetic spectrum (roughly 9,000–14,000 nanometers or 9–14 μm) and produce images of that radiation, called thermograms. The theory is that ALL all objects with a temperature above 0 degrees emits radiation, making thermography a means of measuring just how much radiation is on any specific surface. As radiation increases with temperature, thermography represents temperature variations through image intensity. [4].
On the medical front, clinicians recognize the utility of thermography- in identifying dermal disorders and possible tumors (Fig 3B) including this Invasive ductal carcinoma (IDC), a common form of breast cancer.
Though the FDA does not officially confirm the use of this protocol to replace or supplement the mammogram as a screening tool for any medical condition including the early detection of breast cancer, [
4a], a widening trend in utility within the medical community appears to find more confidence and benefits in the use of
Infrared thermography (IRT). It is found to be a safe, non-invasive alternative to devices such as clinical thermometers, skin physiology via skin temperature. On a 2012 study, IRT has been "successfully used in diagnosis of breast cancer, diabetes neuropathy and peripheral vascular disorders... (and) used to detect problems associated with gynecology, kidney transplantation, dermatology, heart, neonatal physiology, fever screening and brain imaging." [4b]
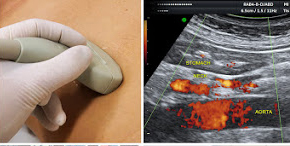
The concept of ultrasound scanning provides the ability to view and study the condition of many vital organs without radiation and without any surgical intervention- instead relying on calibrated sound waves similar to sonar navigation of a submarine. Medical ultrasound devices are known to be one of the safest ways to analyze and diagnose patients. At a frame rate of 10 to 30 images per second, the ultrasound allows us to find any disorder interactively with a hand held probe, while showing an organ's real time activity quantitatively. Today's ultrasound comes with innovative features to offer more quantifiable data gathering- including DOPPLER BLOOD FLOW (to generate imaging of the movement of tissues and body fluids, and their relative velocity to the probe) and 3D/4D Functions (referring to the volume rendering of ultrasound data collected over time)
(OCT) OPTICAL COHERENCE TOMOGRAPHY
Optical coherence tomography (OCT) is an imaging technique that uses low-coherence light to capture micrometer-resolution, two- and three-dimensional images from within optical scattering media (e.g., biological tissue). It is used for medical imaging and industrial nondestructive testing (NDT). Optical coherence tomography is based on low-coherence interferometry, typically employing near-infrared light. The use of relatively long wavelength light allows it to penetrate into the scattering medium. Confocal microscopy, another optical technique, typically penetrates less deeply into the sample but with higher resolution. [5]
THE FUTURE OF MODERN BRAIN MONITORING
Since the advent of ultrasound, the trend in medical device technology is noninvasive data gathering that can peer into the body without cutting or causing any aftereffects. And yet, the brain functionality is still almost totally opaque to modern medicine, the only human organ for which we have inadequate tools and diagnostic tests. In addition, existing tools such as fMRI and PET imaging have historically been unable to test brain functionality during a standard daily routine, with real rather than simulated sensory stimulation and activity.
Our editors are reviewing a brain-scanning innovation by Neurosteer Inc. Their non-invasive device is designed to monitor comprehensive brain health with EEG (Electroencephalography) technology that uses a wearable, medical-grade brain activity monitor for a wide range of medical, wellness and lifestyle applications. The adhesive forehead strip contains 3 electrode sensors that scan brain activity and is connected to a pocket-sized sensor that wirelessly transmits data to the cloud for signal processing, which supports screening, continuous patient monitoring, optimized neurostimulation and drug selection. This unique device is currently undergoing research trials to be confirmed for a set of applications including early detection of cognitive decline, quantifying the effect of tDCS (Transcranial direct-current stimulation) on different patients, quantifying and assessing surgeon performance.
REFERENCES:
1c) "Guidelines for wrist-worn consumer wearable assessment of heart rate in biobehavioral research" -
4b) Source: Pubmed: Medical applications of infrared thermography: A review-